Wild Running & Camping in the Lakes
For the past month we've had the absolute privilege of living under canvas in the…
Plantar fasciitis is a painful foot condition that affects many thousands of people each year. According to the British Medical Journal it accounts for 11% to 15% of all foot complaints requiring a visit to a medical practitioner and occurs in about 10% of regular runners. It’s not surprising, therefore, that during my time as a podiatrist and a distance runner I’ve had more than my fair share of encounters with the condition.
What is Plantar Fasciitis?
It’s a common condition characterised by pain at the insertion of the plantar fascia (the fibrous band you can feel in the arch of your foot when you pull your toes upwards) on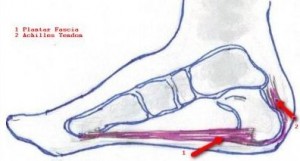 to the calcaneus or heel bone. There are many proposed causes, and it’s likely to be a combination of factors that triggers its onset. Runners suffer more than most as running results in repeated traction of this area as the arch flattens with each foot strike. Despite being termed an ‘itis’ which indicates inflammation, recent findings have suggested that it is instead a degenerative condition very much like the tendinopathy found in the Achilles and patellar tendons, with associated muscle wasting of the intrinsic muscles of the foot. There is some good work currently being done looking at treating plantar fasciitis in the same way as the better-recognised tendinopathies, using high-load strength training to stimulate regeneration of the damaged fibres.
to the calcaneus or heel bone. There are many proposed causes, and it’s likely to be a combination of factors that triggers its onset. Runners suffer more than most as running results in repeated traction of this area as the arch flattens with each foot strike. Despite being termed an ‘itis’ which indicates inflammation, recent findings have suggested that it is instead a degenerative condition very much like the tendinopathy found in the Achilles and patellar tendons, with associated muscle wasting of the intrinsic muscles of the foot. There is some good work currently being done looking at treating plantar fasciitis in the same way as the better-recognised tendinopathies, using high-load strength training to stimulate regeneration of the damaged fibres.
It was my own experiences of plantar fasciitis that shaped my early career. Training for my first marathon was going well until I noticed a niggling pain where the arch of my foot meets my heel. Before long I could hardly walk, let alone run, and watched as my hard-earned fitness began to disappear. I started to do a bit of research and, three months later I’d tried every ‘cure’ I could find, from rolling frozen bottles to calf stretches, with no improvement. I was repeatedly frustrated by the attitude of the GPs I saw. One of them even said to me “if it hurts when you hit it with a hammer – stop hitting it with a hammer” – or in other words, stop running.
Then one day, after months of frustration and no clear answers, the pain suddenly vanished. I’ve heard many people say this is how it goes – suddenly you just realise it doesn’t hurt any more. I went back to training and ran my marathon – but it had got me interested. So interested that I went off and did a degree in podiatry, specialising in running injuries of the foot, and then completed an MSc researching changes that occur in the foot during long distance running.
It was during my year as a masters student that the dreaded niggle appeared again, this time in the other foot. It came and went for a bit and then worsened until I was unable to run at all. This time I was determined to find the answer and set out to test out every treatment I could get my hands on in the name of podiatric medicine. Here’s a rundown of my experiences:
Orthotics
As a musculoskeletal podiatrist I’ve prescribed a lot of orthotics. Unlike many in the profession, however, I don’t tend to go for permanent devices made with a cast – I’ve found these are too heavy and restrictive for most distance runners, with too little evidence based on good quality, long-term studies to back up their use. I’ve seen the changes they effect at the knee and hip and am loathe to simply move the injury up a joint or two. I’ve used customised temporary orthotics successfully many times; they’re great for offloading a structure while it heals or changing foot function slightly in conjunction with a good strength and conditioning programme. Following the theory that the traction caused by the flattening of my arch might be the cause of my injury I made myself a set of temporary orthotics with medial support, designed to control pronation. I found these and some off-the-shelf inserts I subsequently purchased irritated the site of my injury and rapidly became unbearable to wear.
Stretching
There is some evidence that stretching the plantar fascia itself might have a beneficial effect, however I found that although it felt better immediately afterwards there was no longer-term effect.
Night Splints
Highly recommended by internet forums but lacking evidence from good studies the theory is that night splints prevent the plantar fascia from constricting during sleeping. I simply couldn’t sleep with mine on.
Ultrasound
Ultrasound can be used to image the plantar fascia to assist in making a diagnosis, or as a theraputic aid. I had both: the first confirmed that my plantar fascia was thickened in comparison with my non-injured side and the second felt pleasant but had no noticeable long-term effect.
Acupuncture
I’ve heard a lot of good things about the healing powers of acupuncture, however I’d never tried it out myself. There’s definitely a lack of evidence supporting its effectiveness in treating plantar fasciitis. I had the recommended course of treatments but noticed no change in my condition.
Steroid Injection
Eventually, seemingly out of all other options, my GP referred me to the hospital for an ultrasound-guided corticosteroid injection. I was a bit nervous about this, not being a fan of needles and having read that there may be an increased risk of rupture of the plantar fascia following this intervention. The injection itself was one of the most painful experiences of my life, however within a couple of days I was walking around pain-free. I tentatively tried out a run – still no pain. The next day I woke with numbness and tingling down the outside of my foot and pain throughout the foot that meant I could hardly put any weight on it at all. Nerve conduction studies found a minor nerve injury had resulted from the injection – a known risk of the treatment. It took around 6 months for sensation in my foot to return to normal and the plantar fasciitis was back with a vengeance within a week.
Low Dye Taping
Some of the most promising findings in treating plantar fasciitis come from the use of non-stretchy zinc oxide tape to support the arch. Here’s an easy-to-follow set of instructions on applying the tape. Having discovered this taping technique I wouldn’t go back to any other treatment and I’ve used it successfully on many patients and friends with plantar fasciitis. It’s not an instant cure, of course, but if you tape every day you can continue to train as normal until the condition resolves itself. It takes a few attempts to get the taping right, but once perfected it should feel very supportive, without being uncomfortable. Use more tension at the heel than the forefoot and don’t be afraid to add a double layer in the places you want the most support.
Still nowhere near enough is known about plantar fasciitis for there to be any definitive answers, however hopefully the above might help anyone affected to navigate through the maze of advice and opinion that’s widely published online.